
Are you engaged in research? Take one of the projects you’re involved in…
- Is the team lead a white person or a person of color? How about the rest of the team, who are you inviting on it?
- Who are you studying; do they have a real say in the research agenda?
- Who do you cite; do you actively search for and include scholars from underrepresented backgrounds?
- Similarly, who do you invite to give presentations?
I’m talking to myself as much as I’m talking to you; there are so many areas where I should have been more inclusive (more on that later). This Wednesday/Thursday we hold a session (2 time zone options) to brainstorm small steps that we can already take to improve what we do.
Today, I wanted to talk about what motivated our team to organize this session: what we learned from our project on child trauma treatment guidelines.
Clinical practice guidelines are documents that inform clinical practice in several ways. They tell us what current evidence-based practice is, what the best trauma treatments are. They inform practitioners, prospective clients, professional associations, policy makers, program managers, regulatory agencies, and insurers, to name a few.
So they are important and influential. They can support equity and inclusion by means of their recommendations.
While doing an initial exercise of comparing recommendations across various guidelines, we got interested in children’s representation:
- whether children had had a voice in the guideline process (as a ‘consumer’) and
- whether their diversity of cultural backgrounds had been recognized and represented
The full – though short 😊 – commentary is available here (open access). Here is a quick overview of what we found:
Voice:
As far as we could tell from the 14 sets of guidance documents we considered, children or young people had not been actively involved in the development process of the guidelines:
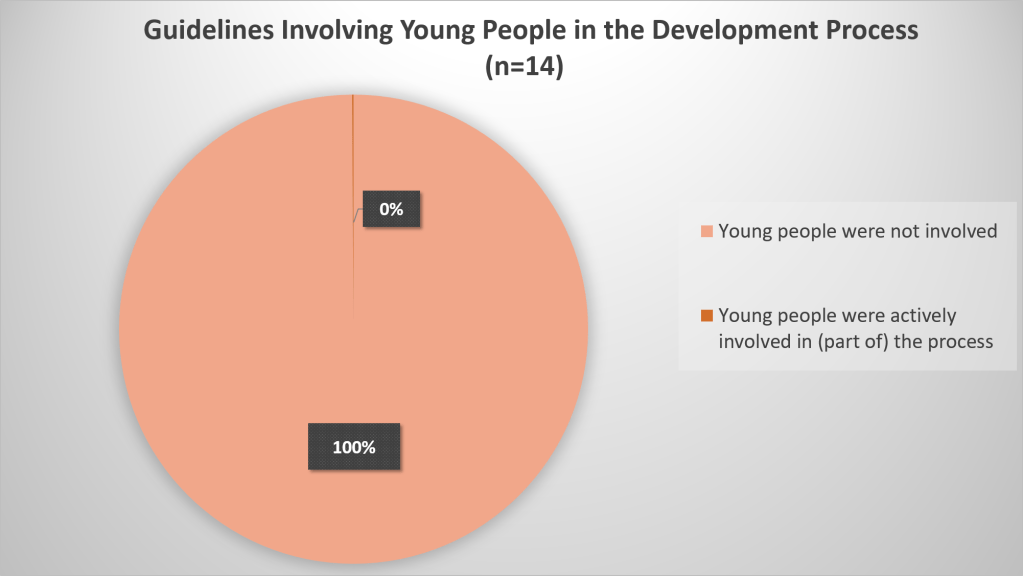
They will have had a voice via the input from child-focused practitioners and researchers but we didn’t find reports of facilitated discussions or consultation with children and/or young people allowing their voice to be heard directly regarding proposed guideline questions, procedures or recommendations.
Cultural background:
Continue reading
